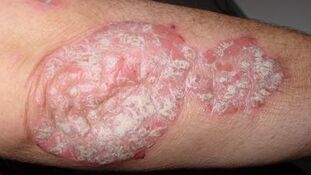
Psoriasis is a long-term chronic skin disease.
The reasons for the development of the disease
Psoriasis occurs due to the pathology of skin cells, when the top layer of the skin dies off within 4-5 days, while normally this time interval is several weeks. The causes of the disease are not fully understood, but doctors identify several factors that provoke the disease:
- Hereditary predisposition - the disease manifests itself at a young age, starting from 15 years, and is more often inherited. If one of the parents has been diagnosed with psoriasis, the child has a more than 50% chance of getting sick.
- Autoimmune conflict - with this type of disorder, the body's immune cells stop recognizing skin cells as part of the body, starting to attack them as foreign elements.
- Nervous shocks - promote the release of hormones into the bloodstream, which leads to metabolic disorders and provokes the development of the disease.
- Disruption of hormonal balance and metabolism.
Psoriasis is not contagious, as there are no infectious agents that can be transmitted.
Psoriasis Symptoms
The main symptoms of the disease are characteristic rashes on the skin, mainly affecting the inner surface of the elbow and knee joints, as well as those areas of the skin that are subject to frequent friction trauma.
Rashes along the edge of the scalp and other less typical sites may also be observed.
Skin rashes appear as patches covered with grayish or white scales. Skin rashes in psoriasis have three characteristic features:
- Stearin spot symptom:Whitish scales peel off easily, resembling candle wax crumbs in appearance.
- Terminal film- after the scales have been removed, a whitish film can be seen under them covering the surface of the spot.
- Spot bleeding- when scratching the spot, the terminal film is removed, the skin papillae are damaged, on which small droplets of blood protrude.
At an early stage, a pale rim is formed around the papule, no peeling occurs at this stage. Pallor around the spot is a vascular reaction of the body to the rejection of the epidermis. The disease is accompanied by severe itching of the skin; when scratching, cracks and minor bleeding are formed on the skin. A secondary infection can join, penetrating through the damaged skin.
In addition to the skin, psoriasis affects the nails, causing fragility of the nail plates, the appearance of a transverse pattern and concave areas.
Autoimmune conflict can affect joints, causing arthritic-like pain, especially in the joints of the fingers.
Types of psoriasis
Psoriasis of the first type occurs in people younger than 30 years old, it is a hereditary disease that mainly affects the skin and has a typical localization.
Type II psoriasis affects people over forty and is not inherited. More often it affects the nail plates and the scalp, the rash is small and tear-shaped. The disease in elderly patients is due to a decrease in immunity against the background of chronic infectious diseases and improper lifestyle.
Clinical studies have shown a link between type 2 psoriasis and alcohol and unhealthy food abuse.
Forms of psoriasis
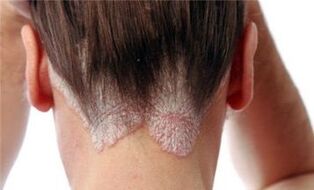
Psoriasis has several forms of varying severity:
- Plaque psoriasis- characteristic papules form on the skin, accompanied by itching and flaking.
- Pustular formis characterized by the appearance of bubbles, reddening of the skin around them, severe itching and burning, is considered a moderate form of the disease.
- Erythrodermais characterized by massive skin lesions, accompanied by oozing and discharge of large layers of the epidermis, is especially difficult to tolerate, often accompanied by pustular lesions and fungal infection.
Stages of psoriasis
The disease develops in several stages:
- The initial stagesignals the onset of the disease, during this period one, less often several, pale spots appear, the skin begins to peel off.
- The active stageis accompanied by severe symptoms, profuse discharge of skin scales, itching and inflammation.
- Stationary phase- indicates remission, peeling at this stage practically stops, instead of a spot, pigmentation or pale areas of pseudoatrophy are formed.
Psoriasis Diagnostics
To make a diagnosis, you must see a dermatologist. The pathology has a clear clinical picture, confirmed by anamnesis and biopsy of skin elements with their subsequent study.
Psoriasis Treatment
The treatment of the disease should be approached comprehensively, at the same time stopping external symptoms and influencing the possible cause of the disease.
Drug therapy
In severe cases, measures are taken to reduce the body's immune attack on its own cells:
- Cytostatics;
- Antihistamines;
- Corticosteroid hormones;
- Enterosorbents and hepatoprotectors are used to restore metabolism.
At the same time, measures are being taken to saturate the body with the necessary vitamins and microelements:
- Silicon is one of the important trace elements responsible for hormone balance and skin health.
- Calcium and vitamin D3 are necessary to bring the disease into remission. Prescribed together to increase calcium absorption.
Local remedies
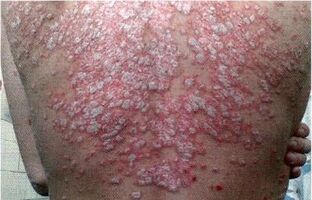
For skin protection, external agents are used in the form of ointments and creams:
- Glucocorticoids, which reduce the immune response, also reduce the symptoms of inflammation, relieve itching and swelling of the skin.
- Salicylic acid and herbal products are essential for moisturizing the skin and protecting against secondary infections.
- Topical cytostatics are used only in the active phase of the disease with its severe course.
Procedures
In order to speed up the healing process, physiological procedures are prescribed:
- Cryotherapy;
- UV irradiation;
- Laser processing.
If necessary, plasmapheresis is performed to purify blood plasma and stabilize cells.
Prevention
If a predisposition to the disease is identified, it is necessary to take a number of preventive measures:
- Lead a healthy lifestyle, stop smoking and alcohol;
- Build a daily routine, avoid stress, rationally approach the organization of the work schedule;
- Follow a diet, avoid excessive amounts of carbohydrates, spices and fatty foods. It is advisable to avoid preservatives and instant foods;
- Spend enough time outdoors;
- Use soap and shampoo with a specially selected pH value, do not use hard washcloths and towels, thoroughly dry the skin after a shower;
- Wear clothes made from natural materials that are not too close to the body;
- Periodically undergo a medical examination, control the level of hormones in the blood, and, if necessary, start early treatment.
Such measures will help maintain healthy skin and significantly improve the quality of life.























