Stages of psoriasis are defined time intervals during which the disease takes on its characteristic features. Many psoriatics mistakenly call the stage a severe or mild form of the disease, but in medical records the term is used in a completely different meaning.
What are the stages of psoriasis?
Psoriasis is recognized as a recurrent skin pathology, in the occurrence of which genetics are to blame. According to dermatologists, at least 2% of the world's population suffers from this disease, which means that the problem is very urgent. During psoriasis, 2 conditions are clearly distinguished:
- Relapse.This term refers to the deterioration of the skin. In relapse, the patient suffers from itching, pain, burning, profuse skin rashes, irritation and discomfort. The situation of the victim is aggravated by insomnia, neurosis and anxiety.
- Remission.This word is used to mean improving the appearance of the skin. With remission, the skin regains its normal color, the redness goes away, and the area of psoriatic plaques is reduced.
The stages of psoriasis partly duplicate the description of remission and relapse, so many dermatologists use these words interchangeably. In clinical practice, 3 stages of psoriasis are described:
- progress stage;
- stationary;
- regression stage.
Considering that we are talking about a cyclical process, the stages sequentially flow into each other and form a continuous course of the disease.
Fact!The stage of progress is considered the most difficult to feel.
What is psoriasis progress?
The progress stage is triggered by a number of triggers, such as the cold season or stress. In some cases, even an experienced dermatologist cannot identify the trigger unambiguously. During the progressive stage, the following happens:
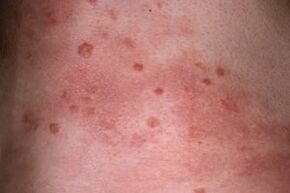
- Psoriatic nodules develop quickly, affect the skin, interconnect in the so-called plaques, which flake and itch. A plaque is an arbitrary-shaped spot, most often round or oval, sometimes with an uneven edge.
- Papules, that is, individual nodules of a psoriatic rash, are lumps on the skin. The edges of the papules do not peel off, and the central part is peeled off. As a large number of dead scales accumulate, plaques begin to rise above the surface of the skin. Puffiness gives them an even more convex and uneven appearance.
- This stage of pathology is characterized by an isomorphic reaction, which consists in exacerbation of rashes in case of skin lesions, scratches, injections, cuts, microtraumas. This phenomenon bears the name of Köbner.
A delayed reaction is characteristic of the progressive stage of psoriasis. In some cases, skin rashes appear about 9 days after exposure to a trigger (such as a food allergen). Typically, a psoriatic rash appears within 24 hours after exposure to adverse factors.
Interesting!95% of psoriatics have some type of food intolerance that can trigger a relapse. To avoid exacerbation, you need to keep a food diary and observe the reaction to different types of food.
Stationary and recessive stages
The stationary stage is the period in the course of psoriasis in which the victim's condition is relatively stabilized. In the stationary stage:
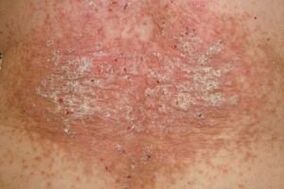
- Psoriatic plaques have a smooth outline. The entire surface of the plaque is covered with a thick layer of scales that easily peel off. Itching and discomfort are moderate. There is no bright red inflamed rim around the papules.
- With microtraumas of the skin, the Koebner phenomenon is not observed, that is, scratching or cutting of healthy skin no longer turns into a psoriatic plaque.
The regressive or recessive stage is characterized by massive lesions in psoriasis. First, a pseudo-atrophic rim can be seen around the papules, and then patients notice a rapid cessation of skin peeling, with the formation of hyperpigmentation plaques in place.
Pathology severity
An additional diagnostic criterion is the assessment of the area of psoriatic lesions. The term "severity" is used to describe it. Dermatologists distinguish 3 degrees of severity of skin disease:
- Easy.Psoriatic plaques occupy 1 to 3% of the total body area. The small size of the affected areas does not mean that the patient is doing well. With psoriasis of the head or face, even a couple of plaques will be enough to cause discomfort and anguish to a person.
- Medium.The volume of psoriatic eruptions occupies from 3 to 10% of the total body area. In this case, the back, chest and external surfaces of the joints, scalp, palms and feet are affected. This prevalence leads to serious intoxication and severe pain. The patient may completely or partially lose his ability to work, the mental state and the state of the nervous system deteriorate.
- Heavy.The disease covers more than 10-15% of the skin surface. According to rough estimates, if psoriasis occupies more than a quarter of the total body area, the likelihood of liver or kidney failure increases many times. Decompensated damage to internal organs can cause the death of psoriasis.
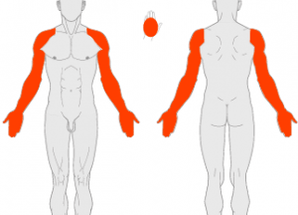
In order to comprehensively assess the severity of psoriasis, a special scale called PASI is used. The scale takes into account:
- percentage of healthy and diseased skin;
- stage of pathology;
- patient's response to drug therapy;
- individual tolerance of psoriasis (mental state, complications from the nervous system and psyche);
- objective data of laboratory tests in dynamics (for example, the volume of uric acid in a blood test).
The diagnosis takes into account all the symptoms that affect the condition of a person with psoriasis. The intensity is reflected in the medical record:
- itching processes of the skin;
- redness;
- puffiness;
- hyperemia;
- skin thickening;
- exfoliation;
- blood flow;
- swelling;
- infections;
- pain syndrome.
On the PASI scale, the volume of skin lesions is described by numbers, from 0 to 72, where 0 is the absence of skin symptoms, and 72 is the large-scale, maximum possible spread of the disease.
Attention!It is important for the patient first of all to know and monitor the signs of an exacerbation. If unfavorable symptoms appear, you should immediately visit a dermatologist, because psoriasis does not always enter the stationary stage itself. A relapse can last for decades.
Treatment of psoriasis depends on the stage
For each stage of the disease, its own set of therapeutic measures has been developed, so the first thing a dermatologist does is determine whether psoriasis is progressing, stabilized or regressed.
How is progressive stage treated
Every psoriasis sufferer guesses that the remission is coming to an end by his own feelings. If itching gets worse, the skin looks worse, and the psoriasis is evidently spreading over the surface of the body, treatment should be started. Therapy for the advanced stage has the following features:
- The patient is engaged in the prevention of further deterioration, strictly adheres to the diet, refrains from triggers of the pathological process (stress, smoking, alcohol).
- For severe itching, antihistamines can be used, an additional benefit of this class of drugs is the removal of puffiness in the area of psoriatic plaques.
- The dermatologist prescribes a wide range of topical treatments to heal, soften and thin the skin. By decision of the doctor, creams, ointments or sprays are selected. Tar soap and solid oil compresses give positive dynamics. You can also apply compresses or apply cosmetics with Dead Sea mud.
The main task at this stage is to stop the exacerbation before the disease enters a prolonged relapse. According to the indications, the doctor selects corticosteroids in injections or in the form of ointments.
Attention!Corticosteroids should be used in a short, intensive course under the supervision of a dermatologist. You can give yourself injections or smear antihistamine ointments.
Stationary and regressive stage therapy
Further actions of the dermatologist depend on the body's response to the selected treatment. The following scenarios are possible:
- Medication has a positive effect. Within 1-2 weeks, psoriasis passes the stationary stage, regresses and remission occurs.
- Medications have no effect. If, after 2-4 weeks from the moment of prescribing the course of drugs, the results are still not visible, this is a reason to change either the list of drugs or the attending physician.
- Medication aggravates. Such dynamics is also possible, especially if the dose or frequency of administration is not enough. The relapse is delayed, psoriatic plaques cover a large area of the body, the person needs hospitalization.
In a medical institution, more powerful therapy is used, for example, hardware blood purification. With a favorable reaction, psoriasis enters the stationary stage, which can last from several days to several months.
Interesting!More than 80% of patients notice the seasonal nature of exacerbations. This makes the disease predictable and allows you to prepare for the onset of a relapse.
The list of drugs for the stationary and regressive stages is exactly the same, but the dosage and frequency of administration are less than for the progressive stage.
10-15 year remission
A competent dermatologist sets himself the following task - to choose such medications and physiotherapeutic agents that will give psoriatic patients the longest possible improvement. At the same time, the patient himself should do his best to promote treatment, avoid triggers and take medication responsibly. If the alliance between the patient and the doctor has developed successfully, then the duration of remission is unlimited. Stable wellness can last 15 years or more.























